By Stan Schneider, CEO, Real-Time Innovations and Small Industry Steering Committee Member, IIC
 It is the 6th leading cause of preventable death in the US.
It is the 6th leading cause of preventable death in the US.
It kills over 50,000 people every year in the US alone, and likely ten times more worldwide. That's like crashing three jumbo jets -- every single day.
It harms one in seven of those hospitalized under Medicare. It costs the US government over $4B per year.
It frustrates caring doctors and nurses every day. The stories tear your heart out: Infacts that will never see their homes. Schoolchildren lost to grieving parents. Grandparents whose wisdom will never again enlighten their families. Even worse, this problem has the unique capability to devastate those same caring professionals who have taken an oath to save lives.
What is this killer? Car accidents? Suicide? Guns? Drug abuse? No, these all kill fewer people. The problem is preventable hospital error. Thousands and thousands of errors occur in hospitals every day. Catching them, or even tracking them, is frustratingly ad hoc. Soon, however, connectivity and intelligent distributed medical systems will dramatically improve this forever. This is the revolution that the Industrial Internet of Things (IIoT) promises for patient safety.
This problem is not new. Thirty years ago, the last major change in health care system technology changed hospital care through a simple realization: monitoring patients improve outcomes. That epiphany spawned the dozens of devices that populate every hospital room: pulse oximeters, multi-parameter monitors, ECG monitors, Holter monitors, and more. Over the ensuring years, technology and intelligent algorithms improved many other medical devices, from infusion pumps (IV drug delivery) to ventilators. Healthcare is much better today because of these advances. But errors persist.
Why? Today, these devices all operate independently. There's no way to combine the information from multiple devices and intelligently understand patient status. Devices therefore issue many nuisance alarms. Fatigued healthcare staff members silence the alarms, misconfiguration goes unnoticed, dangerous conditions go unaddressed. And people die.
As an example, consider the picture in Figure 1. The devices in the picture are infusion pumps. Each administers a drug to a single patient. This picture is in an Intensive Care Unit (ICU); an operating room (OR) needs a similar array. In a heart surgery, for instance, the drugs sedate the patient, stop the heart, start the heart, and more. Of course, there are many more devices, including monitors, ventilators, and more. During surgery, a trained anesthesiologist orchestrates delivery and monitors status. The team has their hands full.
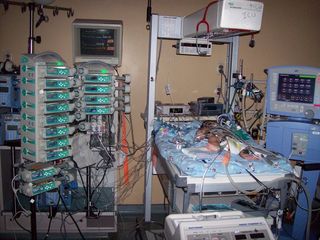
Figure 1: Medical Device Complexity Problem
These fourteen infusion pumps each administer a different drug to a single patient. They are completely independent from each other and the other devices and monitors.
After surgery, the patient must transfer to the Intensive Care Unit (ICU). This is a key risk moment. The drug delivery and monitor constellation must be copied from the operating room to the ICU. Today, the OR nurse calls the ICU on the phone and reads the prescription from a piece of paper. The ICU staff must then scramble to find and configure the correct equipment. The opportunity for small slips in transcription, coupled with the time criticality of the change, is fertile ground for deadly error.
Consider if instead these systems could work together in real time. The OR devices, working with the smart algorithm processor, could communicate the exact drug combinations to the Electronic Medical Record (EMR). The ICU system would check this data against its configuration. Paper and manual configuration produce far too many errors; this connected system eliminates dozens of opportunities for mistakes.
Once in post op, the danger is not over. Many patients use Patient Controlled Analgesia (PCA) systems. The PCA system allows the patient to self-administer doses of painkiller medication by pressing a button. The idea is that a patient with sufficient pain medication will not press the button, and therefore be safe from overdose.
PCA is efficient and successful. Millions of patients use it every year. Still, PCA overdose kills 1-3 patients every day in the US. This seemingly simple system suffers from visitor interference, unexpected patient conditions, and (especially) false alarm fatigue.
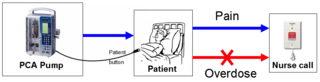
Figure 2. Patient Controlled Analgesia (PCA. The patient presses a button to receive intravenous pain medication. Monitoring is not typically used due to high false/nuisance alarm rate. PCA kills 1-3 people every day in the US.
Connectivity can also help here. For instance, low oximeter readings cause many alarms. They are only likely real problems if accompanied by a low respiratory rate. A smart alarm that checks both oxygen (SPO2) and carbon dioxide (CO2) levels would eliminate many distracting false alarms. An infusion pump that stopped administering drugs in this condition could save many lives.
These are only a few examples. The list of procedures and treatments that suffer from unintended consequences is long. Today's system of advanced devices that cannot work together is rife with opportunity for error. The common weakness: each device is independent. Readings from one device go unverified, causing far too many false alarms. Conditions easily detected by comparing to multiple readings go unnoticed. Actions that can save lives require clinical staff interpretation and intervention.
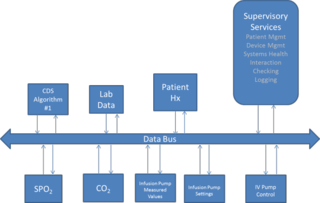
The leading effort to build such a connected system is the Integrated Clinical Environment (ICE) standard, ASTM F2761. ICE combines standards. It takes the data definitions and nomenclature from the IEEE 11073 (x73) standard for health informatics. ICE data communications leverage the Data Distribution Service (DDS) standard. ICE then defines control, data logging, and supervisory functionality to create a connected, intelligent substrate for smart clinical connected systems (Figure 3).
Figure 3. An intelligent Patient Controlled Analgesia system. The supervisor combines oximeter and respirator readings to reduce false alarms and stop drug infusion to prevent overdose. The DDS "DataBus" connects all the components with appropriate real-time reliable delivery.
DDS is an Internet of Things protocol from the Object Management Group (OMG). While there are several IoT protocols, only DDS understands and enforces correct interaction, timing, and operation between participating devices. DDS fits the medical device connectivity problem well. The DD "data centric" model elevates programs to exchange the data itself instead of primitive messages. And, DDS is fast and real-time; it easily handles heart waveforms, image data, and time-critical emergency alerts.
However, the examples above all live in a single room. The real power of the Industrial Internet of Things comes from tying together devices into large intelligent system. Networking medical devices in a real clinical environment with perhaps 1000 beds and 100k devices is truly challenging.
In a real future hospital, information flow will mix slow data updates with fast waveforms. Applications must match data streams to patients, even as physical location and network transports change during transfers between rooms. Devices from many different manufacturers must be coordinated. And security and privacy are critical; each patient’s data should only be available to that patient’s authorized medical team. Finally, cloud-based analytics engines will optimize the system by monitoring patient condition, measuring device utilization, predicting maintenance needs, and even cutting wait times and billing efficiency. This level of data sharing and utilization is the challenge and the promise of the IIoT.
The Industrial Internet Consortium (IIC) fills a unique role in specifying standards for the Industrial Internet of Things. The member companies (130+ strong after less than a year!) are working together to define the system architecture, data management and connectivity strategies, use cases, security designs, and testbeds for the Industrial Internet. RTI is understandably excited and deeply involved; standards like DDS have huge potential to transform the IIoT. You can get a feel for the dynamic energy at IIC meetings by reviewing the slides that we presented at the last meeting on this medical use case here. This is but one of the many important contributions of the IIC.
Hospital error today is a critical healthcare problem. Fortunately, the industry is on the verge of a completely new connected implementation. Smart, connected systems can analyze patient conditions from many different perspectives. They can aid intelligent clinical decisions, in real time. These innovations will save lives.
This technology is only one benefit of the exciting future known as the Industrial Internet of Things. The IIoT will connect many billions of devices together into intelligent systems. It will change every industry, every job, and every life. One of the first applications will extend those lives.